Let’s dive into these interesting facts on how often precum can cause pregnancy, what precum is, the effectiveness of various contraceptives, and more.
Precum (pre-ejaculate fluid) can make people nervous, embarrassed, or downright confused. Most people don’t know what it is or what it does, and there are many misconceptions about it.
First, precum is not the same thing as premature ejaculation. Precum starts oozing around as soon as a man gets all hot and bothered. Oftentimes, it leaks out at various points during or before sex.
Sorry, we couldn’t hold these stats in before the main article:
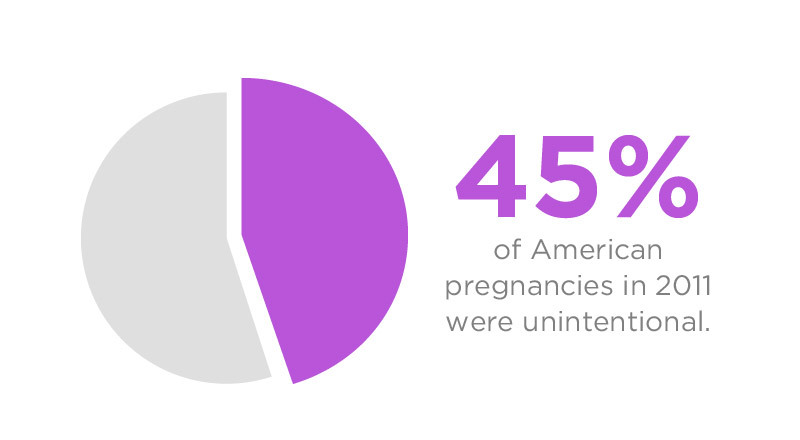
- 45% of American pregnancies in 2011 were unintentional.
- Precum can contain anywhere from no sperm to 5 million sperm (about one-eighth of the sperm in a standard ejaculation).
- When used correctly every time, male condoms are 98% effective.
- 18% of couples who only use the pull-out method experience pregnancy within their first year.
- Most people don’t use the pull-out method perfectly every time, so in reality, it’s only effective 78% of the time. However, if used perfectly, it’s effective 96% of the time.
- When used correctly, the pull-out method (96%) is slightly more effective than female condoms (95%).
What Is Precum and How Often Can Precum Cause Pregnancy?
Precum is sort of like a man’s personal penile lubricant. It doesn’t come from the same glands that make sperm, and it doesn’t serve the same purpose.
Here’s the data on precum and pregnancy:
- Precum (also called pre-ejaculate) is a liquid squeezed out of the penis upon arousal. It’s formed by accessory sex glands different from those that make semen. You cannot feel or control it, and the glands that produce it do not produce sperm. (Web MD, 2022)1
- In normal men, precum volume can range from a few drops to over 5mL. Precum neutralizes the residual acidity of urine in the urethra, which allows sperm to travel safely through. (Journal of Andrology, 2007)2
- Upon arousal, precum is discharged from the penis – typically right before ejaculation. The fluid acts as a natural lubricant. (International Planned Parenthood Federation, 2019)3
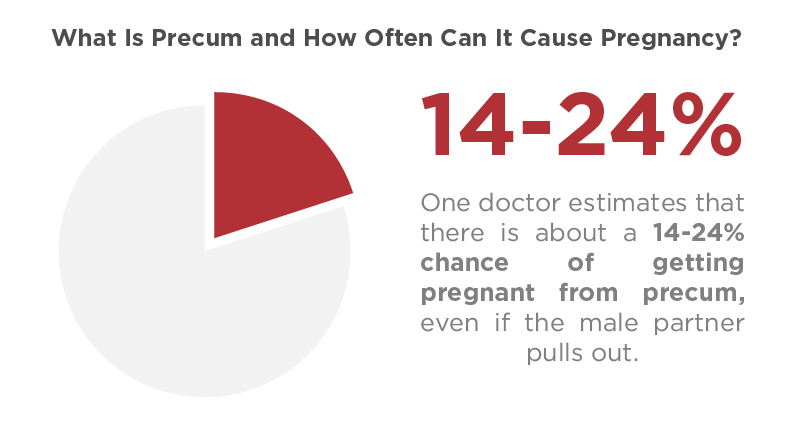
- One doctor estimates that there is about a 14-24% chance of getting pregnant from precum, even if the male partner pulls out. (Seventeen, 2019)4
Does Precum Contain Sperm?

So, is there sperm in precum?
Yes… and no. No two pre-ejaculate fluids are the same, and the sperm content often varies. However, studies conducted in different ways suggest that there may be little or no sperm in precum that leaves the penis a significant time before ejaculation.
Many studies used fluid from men right before orgasm, while others collected fluids during periods of initial or sustained arousal. Each type had different results.
- Standard ejaculated semen fluid contains over 40 million motile sperms. Pre-ejaculate can have anywhere from no sperm to 5 million. (Parents, 2020)5
- One study found that 16.7% of participants had active sperm in their precum. (Journal of the Medical Association of Thailand, 2016)6
- A U.K. study found that 41% of participants produced precum-containing sperm; in most cases, a reasonable amount was active and mobile. (Human Fertility, 2011)7
- One study in which participants (two-thirds of whom had sexual issues) provided precum samples during initial arousal and persistent arousal, but not immediately before orgasm, found that none of the precum contained sperm. (Journal of Assisted Reproduction and Genetics, 2003)8
Is Pulling Out Effective?
The success rate of pulling out varies wildly. You’re almost definitely getting precum in your female partner during sex; whether or not it has any sperm or enough sperm to cause pregnancy is a gamble.
If you pull out perfectly every time (and, let’s be honest, you don’t), there’s a pretty low chance of pregnancy. STIs are a different story, though.
Here’s a look at the data:
- The pull-out method is a birth control method where the man pulls his penis out of a woman’s vagina before he ejaculates. It’s also known as coitus interruptus or the withdrawal method. (Web MD, 2016)9
- One study asked American HIV patients ages 18-25 what they thought about the pull-out method’s effectiveness in preventing pregnancy or the transmission of HIV: (AIDS Patient Care and STDS, 2019)10
- 40% of respondents reported using withdrawal for both HIV and pregnancy prevention.
- 9.5% reported only using withdrawal for HIV prevention.
- 48% reported only using withdrawal for pregnancy prevention.
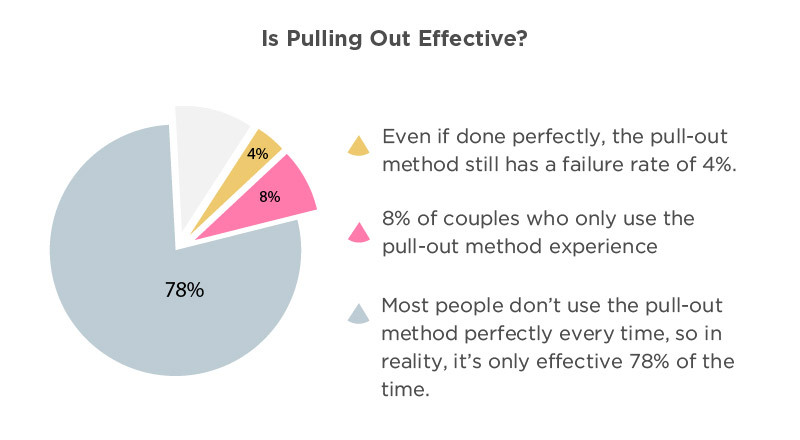
- Even if done perfectly, the pull-out method still has a failure rate of 4%. (Contraception, 2014)11
- 18% of couples who only use the pull-out method experience pregnancy within their first year. (Contraception, 2014)11
- Some people pull out and use condoms during sex. This helps prevent sperm (including precum) from entering the vagina and gives extra protection against pregnancy if the condom breaks. (Medical News Today, 2021)12
- Most people don’t use the pull-out method perfectly every time, so in reality, it’s only effective 78% of the time. (Planned Parenthood, n.d.)13
- When used correctly every time, male condoms are 98% effective. (National Health Service, 2017a)14
- If used correctly every time, female condoms are 95% effective. (National Health Service, 2017b)15
- Using male condoms has the following advantages and disadvantages: (American Pregnancy Association, 2013)16
- Pros:
- It is one of the few forms of birth control that provides any reduction in the transmission of sexually transmitted diseases.
- Condoms are inexpensive and easily obtained.
- No side effects unless you are allergic to latex.
- You do not need a prescription.
- Condoms are small, easy to carry, and disposable.
- Cons:
- Some men complain condoms dull sensations.
- May be considered an interruption during intimate foreplay.
- Requires consistent and diligent use.
- Typical use has a failure rate of approximately 14%.
- It places more responsibility on the male partner.
- Pros:
- The use of female condoms has the following advantages and disadvantages: (Web MD, 2021)17
- Pros:
- You can put one in up to 8 hours before sex, so you don’t have to interrupt the mood.
- Women can choose to use them if their partners don’t want to wear a condom.
- They aren’t made of latex, which irritates some people’s skin.
- They stay in place if your partner loses their erection.
- You put them in before sex, so you don’t have to stop what you’re doing as you do with a male condom.
- You don’t have to remove them right after sex, so you can enjoy the moment more.
- Cons:
- They can slip out of place during sex.
- They can irritate your or your partner’s skin.
- They might make the sensation of sex less intense. If this is a problem for you, try to make putting in the condom part of sex play.
- They’re slightly less effective at preventing pregnancy and STDs than male condoms.
- They can be noisy, but you can use more lubrication help or put it in early, so it has time to warm up to body temperature.
- They cost more than male condoms.
- There’s only one size.
- Pros:
- Using the pull-out (withdrawal) method during sex has the following advantages and disadvantages: (American Pregnancy Association, 2022)18
- Pros:
- Withdrawal can be used every time.
- Withdrawal may be added to other forms of birth control to increase its effectiveness.
- Withdrawal is free.
- Withdrawal does not require a prescription or manipulation of some mechanism.
- Cons:
- Withdrawal is not considered the most reliable form of birth control.
- The woman must have complete trust in the man’s ability to withdraw.
- Pre-ejaculation, which may contain sperm, occurs without the man’s knowledge.
- Some men have difficulty timing their withdrawal.
- Pros:
Precum and Birth Control
Precum can cause pregnancy, even if it isn’t particularly common, but how effective is birth control against it?
Different birth controls have different success rates. Since nearly half of all American pregnancies are unintentional, it’s safe to say that they aren’t all perfect.
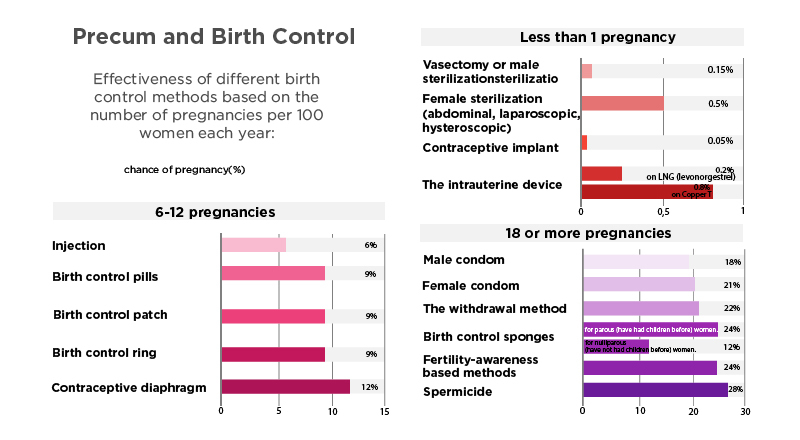
- The CDC has provided the following data on the effectiveness of different birth control methods based on the number of pregnancies per 100 women each year: (Centers for Disease Control and Prevention, 2016)19
- Less than 1 pregnancy per 100 women in a year:
- Vasectomy or male sterilization
- 0.15% chance of pregnancy
- Female sterilization (abdominal, laparoscopic, hysteroscopic)
- 0.5% chance of pregnancy
- Contraceptive implant
- 0.05% chance of pregnancy
- The intrauterine device
- 0.2% chance of pregnancy on LNG (levonorgestrel)
- 0.8% chance of pregnancy on Copper T
- Vasectomy or male sterilization
- 6-12 pregnancies per 100 women in a year:
- Injection
- 6% chance of pregnancy.
- Birth control pills
- 9% chance of pregnancy.
- Birth control patch
- 9% chance of pregnancy.
- Birth control ring
- 9% chance of pregnancy.
- Contraceptive diaphragm
- 12% chance of pregnancy.
- Injection
- 18 or more pregnancies per 100 women in a year:
- Male condom
- 18% chance of pregnancy.
- Female condom
- 21% chance of pregnancy.
- The withdrawal method
- 22% chance of pregnancy.
- Birth control sponges
- 24% chance of pregnancy for parous (have had children before) women.
- 12% chance of pregnancy for nulliparous (have not had children before) women.
- Fertility-awareness based methods
- 24% chance of pregnancy. –
- Spermicide
- 28% chance of pregnancy.
- Male condom
- Less than 1 pregnancy per 100 women in a year:
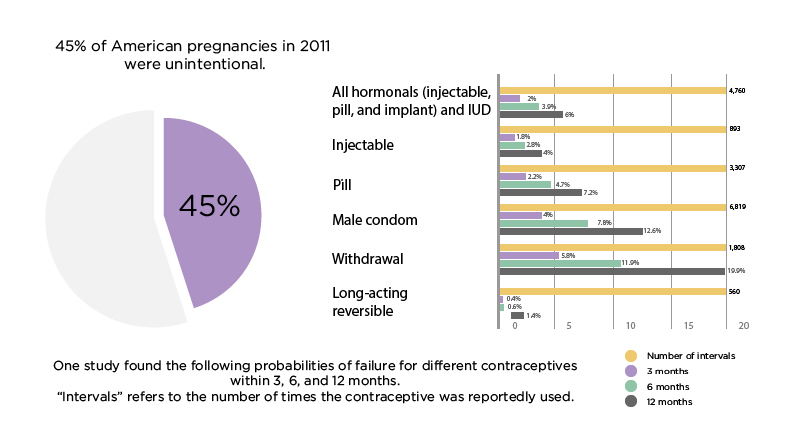
- 45% of American pregnancies in 2011 were unintentional. One study found the following probabilities of failure for different contraceptives within 3, 6, and 12 months. “Intervals” refers to the number of times the contraceptive was reportedly used. (Perspectives on Sexual and Reproductive Health, 2017)20
- All hormonals (injectable, pill, and implant) and IUD
- Number of intervals – 4,760
- 3 months – 2.0% chance of pregnancy.
- 6 months – 3.9%
- 12 months – 6.0%
- Injectable
- Number of intervals – 893
- 3 months – 1.8%
- 6 months – 2.8%
- 12 months – 4.0%
- Pill
- Number of intervals – 3,307
- 3 months – 2.2%
- 6 months – 4.7%
- 12 months – 7.2%
- Male condom
- Number of intervals – 6,819
- 3 months – 4.0%
- 6 months – 7.8%
- 12 months – 12.6%
- Withdrawal
- Number of intervals – 1,808
- 3 months – 5.8%
- 6 months – 11.9%
- 12 months – 19.9%
- Long-acting reversible (IUD and implant)
- Number of intervals – 560
- 3 months – 0.4%
- 6 months – 0.6%
- 12 months – 1.4%
- All hormonals (injectable, pill, and implant) and IUD
Do Ovulation and Menstruation Affect the Chance of Pregnancy?

If your partner insists that she can’t get pregnant at a certain time of the month, you might be justifiably skeptical. Female fertility fluctuates with their ovulation cycle.
There are times when the chance of pregnancy is close to zero, but there are also times when the chance is higher than usual.
- Ovulation is when the ovary releases an egg to be fertilized. Women are most likely to get pregnant from sex from three days before up to the day of ovulation. (Office on Women’s Health, 2021)21
- It’s possible to get pregnant 12-24 hours after ovulation. Sperm can live up to 5 days in a woman’s body, and they take about 6 hours to reach the fallopian tubes. A woman can quickly become pregnant if sperm is present when the egg is released or shortly after. (American Pregnancy Association, 2021)22
- Chances of getting pregnant rise and fall throughout a woman’s ovulation cycle. The average cycle is 29 days, but this can vary from 20-40 days or longer. (Healthline, 2016)23
- There’s almost no chance that a woman will get pregnant 1-2 days after she starts bleeding. The likelihood increases each day after that, even if she’s still bleeding. (Healthline, 2016)
- A woman has only about a 9% of getting pregnant approximately 13 days after starting her period. (Healthline, 2016)
Precum and Sexually-Transmitted Infections (STIs)
Pregnancy isn’t the only thing you have to worry about from precum. STIs are sneaky little bacteria or viruses that just love to spread.
Even in precum, they wriggle and procreate and try to find a new host.
- Precum can transmit the following diseases: (Very Well Health, 2021)24
- HIV
- The human immunodeficiency virus (HIV) lives in blood, vaginal fluid, semen, breast milk, and precum.
- Chlamydia
- Chlamydia is the most common STI in the U.S. The bacteria that cause it can live in vaginal fluid, semen, and precum.
- Gonorrhea
- Gonorrhea is another common bacterial infection transmitted through semen, vaginal fluid, and precum.
- Hepatitis B
- Hepatitis B is a highly infectious virus that affects the liver. It is the only strain of hepatitis that can be transmitted through precum.
- HIV
- One study of HIV-positive men on highly active antiretroviral therapy (HAART) found that 1 of 8 men tested had HIV in his precum. However, this does not mean that it is safe to have unprotected sex with HIV-positive men. (AIDS, 2016)25
Conclusion
Pre-ejaculate fluid, also known as precum, is a natural lubricating fluid that balances the pH levels in a man’s urethra when he gets sexually excited so that his sperm isn’t harmed by residual acidity.
Precum can contain millions of sperm or no sperm at all. It can carry STIs and is secreted during arousal, sexual activity, and before ejaculation. Male condoms are the most effective non-invasive protection against both pregnancy and STIs from precum.
Male vasectomies and female contraceptive implants are the most effective ways to avoid getting pregnant. There are also certain times during a woman’s ovulation cycle when pregnancy is highly unlikely.
Precum may have a significantly lower chance of causing pregnancy than a full ejaculation load, but it’s still something to be conscious of when having sex.
Footnotes
- Web MD, 2022. A medically-reviewed article on the definition of pre-ejaculate (precum), how it works, and whether or not it can cause pregnancy.
- Journal of Andrology, 2007. A medical article on the biological function of pre-ejaculation and the rare cases of over-production of precum.
- International Planned Parenthood Federation, 2019. An article on the biological function of pre-ejaculate and its chances of causing pregnancy.
- Seventeen, 2019. An article on the chances of getting pregnant from pre-ejaculate using input from Dr. Natasha Bhuyan, MD.
- Parents, 2020. An article on the chances of getting pregnant from precum citing input from Dr. Mike Hsieh, MD, urologist, and director of the Men’s Health Center at UC San Diego Health.
- Journal of the Medical Association of Thailand, 2016. A study on the presence of sperm in pre-ejaculate fluid in 42 Tha men.
- Human Fertility, 2011. A study on the presence of sperm in pre-ejaculate fluid using data from 28 men in the U.K.
- Journal of Assisted Reproduction and Genetics, 2003. A study of the presence of sperm in pre-ejaculate fluid using data from 8 men with either excessive precum or premature ejaculation and 4 men with no sexual complaints.
- Web MD, 2016. A medically-reviewed article on the effectiveness of the pull-out method of birth control as well as its advantages and disadvantages.
- AIDS Patient Care and STDS, 2019. A study on the effectiveness of the pull-out method in preventing pregnancy and the transmission of HIV using data from 88 HIV-positive American youths aged 18-25.
- Contraception, 2014. A study of the prevalence of different contraceptive methods used by 4,634 American women ages 18-39.
- Medical News Today, 2021. A medically-reviewed article on the chance of pre-ejaculate causing pregnancy and the factors that affect it.
- Planned Parenthood, n.d. A small article on the effectiveness of using the pull-out method as birth control.
- National Health Service, 2017a. A comprehensive article on the use of male condoms as birth control, how to use them, and their advantages and disadvantages.
- National Health Service, 2017b. A comprehensive article on the use of female condoms as birth control, how to use them, and their advantages and disadvantages.
- American Pregnancy Association, 2013. An article on the functionality, advantages, and disadvantages of the use of male condoms.
- Web MD, 2021. A medically-reviewed article on the functionality, advantages, and disadvantages of the use of female condoms.
- American Pregnancy Association, 2022. An article on the use, advantages, and disadvantages of using the pull-out (withdrawal) method.
- Centers for Disease Control and Prevention, 2016. A statistical report on government-recommended contraceptive use from the CDC.
- Perspectives on Sexual and Reproductive Health, 2017. A study on the failures of different contraceptives in the U.S. using data from 6,683 American women.
- Office on Women’s Health, 2021. An article from the U.S. Department of Health & Human Services on women’s menstruation cycles.
- American Pregnancy Association, 2021. An article on ovulation and the chance of getting pregnant after the ovulation period.
- Healthline, 2016. An article on how menstruation affects a woman’s chances of getting pregnant during her period.
- Very Well Health, 2021. An article on pre-ejaculate fluid (precum) and the diseases that can be transmitted by it.
- AIDS, 2016. A study on the presence of HIV in pre-ejaculate fluid in 60 American men using highly active antiretroviral therapy (HAART).